The battle against the disease becomes all the more difficult
Sakshi Kuchroo and Geetanjali Minhas | June 1, 2016

We ring the doorbell, the door opens slightly and we quickly step inside a cramped two-room flat in Delhi. Raju gives us a furtive look and shuts the door to avoid prying eyes. Before we can talk to him about his serious health condition that has been haunting him and his family for years, he tells us to wait and steps out, possibly to make sure no one followed us to his home.
His wife, in her 30s, covers her face as if to keep a secret. She immediately pulls her two kids inside the kitchen, though they want to stay by their father’s side.
“You can let them stay here. We would be here for 15-20 minutes,” we say to make her comfortable, but it isn’t working. She doesn’t answer us and walks back to her kids.
Raju, 39, is a sweeper at the National Institute of Tuberculosis and Respiratory Diseases (NITRD), a premier TB hospital in Delhi. Located at a stone’s throw from Qutb Minar – a 13th century brick minaret, the hospital is running as an autonomous institute under the ministry of health and family welfare. Raju’s flat is within the hospital premises, so he can be called on duty any time of the day, or night.
To reassure him, we tell Raju that we had followed his instructions – of entering from the rear gate to avoid attracting attention. “I wasn’t sure if I should call you here. Naukri pe khatra na aaye, bas (my job shouldn’t be in jeopardy),” he says. We again promise to keep his identity confidential. But he still looks uneasy. “Humare kayi saathiyon ko TB ho gaya, aur kayi mar gaye (Many of our colleagues had contracted TB and many died),” Raju says while making his way to the kitchen. As we settle on the cream-coloured worn-out sofa, torn at the edges with heavy depressions on the seats, we hear Raju reassuring his wife. He offers us chilled water. As he hands over the glass of water to us, we can see him sweating even under a furiously spinning ceiling fan. We ask him if he is wary of us. “Nahi madam. Bimar rehtey hai is liye (No madam, this is because of my illness),” he says in a shaky voice.
“People like us meet the same fate. Humein koi puchhne wala nahi hai (There is nobody to ask us about our welfare),” he says with an air of fatality.
As a safai karamchari, or janitor, Raju is responsible for maintaining cleanliness in the wards and looking after the personal hygiene of in-patients.
Raju’s day begins at 7 am. From changing bedsheets and clothes of TB patients to dumping their mucus and excreta, his work continues till 2 pm. He is paid Rs. 8,000 a month.
Raju was around 14 when his mother suffered a serious eye injury and had to retire. “She was cleaning the toilets in the hospital when acid accidentally went in her eyes,” Raju recalls. The hospital employed him in her place, 25 years ago.
All was going well – till 1993. That year, Raju’s world turned upside down when he kept coughing for days, had fever, felt tired and couldn’t work properly. “After going through all the tests, I was told that I have TB in my chest. I kept asking for leave but nobody heard me. I was instead told to attend to the patients,” he says with a painful countenance.
“I didn’t know the rules then. It seems the hospital was supposed to give me a three-month paid leave since I had contracted the disease at my workplace. But, they kept deducting my salary for absenteeism as I wasn’t able to work. When I came to know about the rule, I wrote an application; again it took many days for my supervisor to act on it,” Raju says.
The World Health Organisation (WHO) guidelines make it clear that workers like Raju who get exposed to TB-causing bacteria at work should be given special treatment by the employer – regular screening for infection and in case of infection, the patient is to be admitted to an isolated ward. Also, for the first-time TB patients like Raju, the WHO and the health ministry guidelines state that they should receive six months of drug treatment, including two-month intensive treatment.
However, Raju was kept in a ward with other patients who already had multiple-drug resistant TB (MDR-TB) – one of the most serious forms of tuberculosis, as the name suggests. “The ward where I was admitted had all kinds of patients, including the ones who were only suffering from a respiratory disease and not TB. I later realised that all of us had been exposed to TB’s deadlier forms.”
In 1994, clinical tests showed that Raju was free from TB. But it wasn’t the end of his misery. In 2012, Raju was detected with the more dangerous MDR-TB. This type of tuberculosis is caused by bacteria that become resistant to the two most powerful first-line anti-TB drugs – Isoniazid (INH) and Rifampin (RMP). MDR-TB does not respond to the standard six-month treatment regime and needs at least a two-year therapy. The drugs used for treating MDR-TB are quite expensive – easily running over Rs.10,000 a month.
“The second time when I was detected with TB, they admitted me [in hospital] only for 10-15 days and then sent me home. I pleaded with them that I was still infected and since I had my child at home, I didn’t want him to get infected as well,” he says.
However, the hospital management turned a deaf ear. They allegedly told him that they needed him to make way for patients who had paid money to get admitted. “Madam, we are class-IV workers. Why will they care for us?” asks Raju.
“For years, I have been begging the management to change my duty. I have passed 10th standard and I have the necessary experience to be appointed as a supervisor. Main ward ki safai kar nahi sakta tha, par karva toh sakta tha (I might not have been able to clean the ward myself but I could have supervised others to do it),” he adds.
It has been a year since Raju got cured. But he has a nagging feeling that the disease will strike him again. “Many of my colleagues have died like this. Mark my words, I will also die serving them [TB patients] and they [hospital management] will not change,” he says with moist eyes.
TB infection, by and large, spreads through coughing, sneezing and even speaking. During such actions, fine particles called aerosols containing bacteria are thrown into the air. Those in the vicinity inhale these and catch infection. Symptoms include chest pain, chronic cough, cold, fatigue, fever, loss of appetite, weight loss and excessive sweating.
According to WHO’s latest global TB report, “This occupational risk is at alarming proportions in the low- and middle-income countries like India, because of increased exposure and lack of preventive measures.” TB is the third largest killer in India, after cardivascular and respiratory diseases, accounting for every tenth death.
But the government makes no bones about the rising cases of healthcare workers (HCWs) – doctors, nurses and lowest paid employees like Raju – getting infected with TB at their workplace.
Dr Sunil Khaparde, deputy director general, TB, in the union ministry of health, candidly told Governance Now: “About 50 percent of the staff of the Sewree TB hospital in Mumbai has been infected with the disease in the last five years. It’s definitely a matter of grave concern. Similar is the case with the Lala Ram hospital in Delhi [which has been renamed as NITRD].”
Some 1,500 km away from Raju, Lalit Tamboli forms a miniscule part of the high percentage of the TB-infected hospital staff. Tamboli lies on one of the dozen-odd beds lined inside a ward of the crowded GTB hospital in Sewree neighbourhood of Mumbai. Spread across 45 acres of land, it is Asia’s largest TB hospital – perhaps too large to pay Tamboli much attention. With a staff strength of about 1,200, this hospital on average receives 200 patients daily in its OPD and admits 60 for treatment.
In 2010, Tamboli got the job of a sweeper in the operation theatre of a municipal hospital. Work was going as usual when in 2012 he started getting recurring fever, had weakness and body pain and subsequently skipped work. A month later, upon joining back work, he was referred for various tests as per the prevailing practice of the hospital. He was told he had normal TB and was further referred to the revised national tuberculosis control programme (RNTCP) health post near his home where he was prescribed a six-month course of medicines. RNTCP is a government initiative and as per the national strategic plan (for tuberculosis control) 2012-17, the programme aims to make India TB-free and achieve universal access to TB control services. But Tamboli soon realised that its highly ambitious goals looked good only on paper, since six months later he again started feeling feverish and had the same symptoms as earlier.

The National Institute of Tuberculosis and Respiratory Diseases
This time, he went to the GTB hospital where he was admitted for about two weeks. Thereafter he returned to work. And yet in 2015, he was again admitted in the GTB hospital. Doctors there advised him to bring his past reports to determine the category of TB he was suffering from. After reading his reports, doctors told Tamboli to continue with the same medicine he had been taking earlier.
A few months later, when Tamboli felt better, he rejoined duty at the municipal hospital; it was just the beginning of his struggle. Tamboli was told by his employer to get a fitness certificate for which he again had to make rounds of the GTB hospital. Once again, Tamboli had to go through the entire process of undergoing several medical tests. But this time, he was told that he had MDR-TB and that he was taking the wrong medicines all this while. A worried Tamboli spent most of his time inside the GTB hospital but every time he was told to meet a different doctor.

Patients wait at a bus stop outside the TB hospital in Delhi
He was finally admitted in the hospital, yet again. He could not complete his probation period of three years as a sweeper and his file was sent to the Brihanmumbai Municipal Corporation (BMC) to order his sacking. Though he has received a stay certificate on the grounds that he was admitted for treatment, it does not assure him a salary. A forlorn Tamboli is waiting for his leave certificate that will authenticate that he is a BMC employee. Without a source of income for a long time, he is now looking for a job and is keen to admit his child to school. “NGO people have advised me to stay calm, eat proper food and take medicine on time,” he says with little hope.
Kishore Kumar, 50, is another hospital staff member who ended up as a patient. Kumar was lucky as after being detected with MDR-TB, he was given leave from work. But not lucky enough – the medicines he took triggered severe side effects. Kumar started out as a ward boy at the GTB hospital 22 years ago and was promoted to a ward assistant in 2013. In between all this, TB caught up with him in 2005. He was treated but got a relapse of MDR-TB in 2014. Kumar expected to get the benefits entitled to him from the hospital. He did get some, but with an unwanted cost. Put on a wrong medication, his skin colour changed to camouflage brown. His knees pained and he found it difficult to hear.
Sanjay Sonawane’s sorry tale is quite similar. As patients are prescribed to take bed-rest for at least a few weeks, maintaining hygiene is an important part of their daily routine. Here, Sonawane, 51, comes to their help. A barber at the GTB hospital, Sonawane’s interaction with TB-infected patients is high, and so are the chances of him being infected. He has contracted the disease twice, in 2005 and 2013. He too suffered from the side effects of the medicines. “Firstly, I was not provided medicines regularly, and when I bought those from outside, my skin colour changed [into charcoal brown with an eerie tinge of red].”
Dr Rajendra Nanaware, former medical superintendent at the GTB hospital, says that while in the first stage the cure rate is more than 95 percent, if the drug is not administered properly the patient may move into advanced stages like MDR or XDR-TB (extensively drug resistant-TB) or even TDR-TB (totally drug resistant-TB). In TDR-TB, the survival rate is less than 40 percent.
While Sonawane has rejoined work, his salary for four months has not been paid. He says he takes home Rs. 20,000 after deductions from a total salary of Rs. 30,000 every month.
Till recently, if employees had not completed three years of probation period, they were not eligible for leave, says Pradeep Narkar, secretary of Municipal Mazdoor Union. “After we staged a dharna and the issue was raised in the state assembly, grant of medicines and leaves was made possible.”
He adds that as per the recommendations of the infection control committee of the BMC and also of its standing committee, those HCWs who contract MDR-TB and more serious variants should be given paid leave for 24 months by the hospital. However, the January 2016 circular released by BMC, which comes in effect retrospectively from 2013, only provides for nine months’ leave.
But the ground reality is completely different. The staff struggles to get leaves, and even if they get some, their salary is cut. The situation in Delhi is worse. The NITRD usually gives just three months of leave to its staff. Raju got only that much, and that too after much struggle.
Dr DJ Christopher, professor and head, department of pulmonary medicine, Christian Medical College, Vellore, however, has a different take on the debate over leave. He says that only when workers have infection do they need to be given a break from work. Once they are non-infectious and their symptoms reduce, they can return to work as it is not practical and sustainable to send away employees on leave for as long as 24 months.
But before leave can become an issue, why allow TB to spread in the first place? It is clear that a hospital staffer has to work in close proximity with TB-infected patients. Still, preventive measures can be taken. The office of Dr Sunil Khaparde is working on preparing a set of guidelines for hospitals across the country to minimise the risk to HCWs of contracting TB at work. However, Khaparde says that the serious problem is not just a medical one but also linked to development and society. “Our frontline healthcare workers are the backbone of the fight against TB. So, it’s very important that the hospital management takes complete care of its staff,” he says.
The proposed guidelines include a more rigorous screening of HCWs for TB infection, decongestion of TB wards and compulsory wearing of masks for caregivers. Till 2010, the GTB hospital did not follow the mandatory norms like the use of surgical masks, N-95 respiratory masks and adequate air ventilation which obviously led to higher rate of infection among healthcare workers, says Dr Nanaware.
“After 2010, there was an increase in infection in all categories. After our sustained protests they started providing us simple masks. One of the major issues we raised was that the steel container with lid for spitting sputum, called ‘chati’, is not being cleaned properly and therefore poses danger to workers’ health. Currently, sputum is disposed of along with chemicals by flushing it down the toilet or throwing it in the drain. The old practice of using sterilisation machines was discontinued though it was recommended by the infection control committee,” says Narkar.
As an alternative and safer method, Narkar says sputum could be collected in a disposable pouch and burned in a machine or thrown in a boiler. “If proper care is taken for safe disposal of sputum, infection can be controlled and the government can also save a lot of money. A patient usually buys medicines worth Rs. 10,000-12,000 per month for treatment. If the BMC’s budget runs into more than Rs. 37,000 crore [as it is for the current financial year], these machines would not pinch BMC’s pocket as they cost only Rs. 4-5 lakh. But people [in the BMC] who practically have no idea and are not privy to the situation at the ground level take decisions,” he adds.
Dr Damodar Bachani, deputy commissioner, ministry of health and family welfare, favours imparting health education and awareness to the hospital staff as a key preventive measure. “All the staff members are trained but they are very lenient in taking precautions because they think they won’t get the infection. There have been cases wherein a surgeon goes for operation without sterilisation and nurses don’t wear masks. So, counselling is required to make them understand that they can’t be so ignorant regarding their safety.”
Sometimes, the staff face the kind of problems which are apparently not related to TB infections but exacerbate the already bad situation. For instance, non-availability of quality food. Prakash Devdas, president, Mumbai Mahapalika Arogya Seva Karmachari Sanghatana, a body representing municipal nurses and doctors, says it took five years for the management to agree to their demand of a canteen at the GTB premises. “Since the hospital was away from commercial establishments, nursing staff found it difficult to go out and eat. This is despite doctors telling me that a person with an empty stomach is more prone to infection from TB patients. Then why were they not providing food? Finally, they sanctioned Rs. 25 per day for their meals which is a mockery considering crores of rupees allocated towards the state health budget.”
READ: Interview with Blessina Kumar from Global Coalition of TB activists
As per the findings of a survey done by the Christian Medical College, Vellore, two percent of the resident doctors in north India have contracted TB, that is, 11.2 new cases per 1,000 persons crop up every year. The survey also found that the incidence of TB among resident doctors was 10 times higher than that for India. And as per RNTCP’s 2015 report, one-fourth of the global TB cases occur in India. In 2013, out of the estimated global annual incidence of 9 million TB cases, 2.1 million were estimated to have occurred in India.

Patients inside a ward of GTB hospital
Though the ministry is bracing for the challenge, the administrators of hospital are not even ready to accept the problem of HCWs getting TB, leave alone making efforts to prevent it.
Dr Gita Nataraj, professor, microbiology, the KEM and GTB hospitals, and member of the infection control committee, plays down the threat of TB to HCWs. She says, “Healthcare workers, too, get infected just like any other person. There is a possibility that they catch the infection outside the hospital. There is no evidence to prove that workers acquire infection from inside the hospital.”
Dr Rohit Sarin, director, NITRD, too remains in denial. “It’s not like that there is a rise; it is just that awareness about the infection is more. Healthcare workers are prone to infections. It is just that the number of people infected [with latent TB] is more, it is not necessary for them to have the disease as well,” he says.
He categorically denies Dr Khaparde’s claims and says that none from his staff has been infected recently. “We take full precautions here. None of our workers have been infected in the past 5-10 years. We hold regular counselling and annual checkups for them,” he adds.
Ironic as it may sound, he blames HCWs for hiding their disease for the fear of social stigma and thereby prolonging the treatment.
We ask Dr Sarin for data on HCWs contracting infection. He says that we should check it with the hospital management. He asks a doctor named Khalid to take us around the hospital.
And thereon, starts our curated and guided tour of the hospital.
The hospital looks spick and span; he makes us speak to a few chosen members of the staff. “She’s from the media. Tell her what precautions you take in the hospital,” Dr Khalid asks Babita, one of the TB health visitors. She says, “We teach the staff all about TB. And they listen to us and follow all the instructions. It is difficult to teach the staff in AIIMS because they don’t listen but here everything is good. There is no one who is infected with TB in this hospital.”
After moving around in the corridors and wards for about 20 minutes, Dr Khalid ushers us to the hospital gate and bids a firm goodbye. He too parries question on exact data of infection among HCWs. We tried to get in touch with the hospital management through email and telephone; there was no response.
Shambhu Kumar Singh, leader of the Employee Union of NITRD, gets angry when we tell him that Dr Sarin had told us that HCWs keep the disease under the wraps. “Jhuth boltey hain. Aadmi ko agar marne ki ichha hogi tab hi chhupaega aur memsahib, vishwas kijiye, hum marna nahi chahtey (He is lying. A person will lie only if he has a wish to die and madam, trust me, we don’t want to die).”
He alleges that the management refuses to grant leave to TB-infected staff and exploits their lack of knowledge about rules and regulations. “They might hold counselling for patients every month or two, but a sweeper or a ward boy is never welcome there. In fact, on World TB Day (March 24) this year, they ordered all the sweepers to leave the venue of the function. They don’t consider them valuable,” he claims.
Seconding Singh, Shyamlal, a senior safai karamchari, says, “Doctor logon ko jo salah deni hoti hai, woh un patient log ko dete hai jo paisa dete hai, humse koi baat nahi karta (Doctors give advice only to those patients who pay money, they don’t talk to us).” Shyamlal was detected with TB in 1993.
We visit Shyamlal’s house where his wife Poonam is eager to speak up. “He has MDR-TB. Doctors have strictly told me to stop him from smoking and drinking but he doesn’t listen. He is addicted to it. How will he get better? It is his fault too,” she says angrily.
Shyamlal has his own story: “Hospital wale admit nahi karte. Humein dawai bhi time pe nahi milti. Woh kya salah dengey (The hospital refuses to admit us and we don’t even get the medicines on time. What advice would they give)?” he asks, looking at Poonam.
Shyamlal is supposed to get drugs free of cost from government hospitals. However, each time he has gone there, he is told that stocks are over and he should come later. He says, “Despite making many rounds, we never get the medicine. Since they are very expensive, we can’t think of buying them.”
Going by Shyamlal’s version, the claim that hospital provides counselling seems a sham. He has not been made to realise that not taking medicines will further complicate his health condition. Shyamlal, who has been serving TB patients for 28 years, has given up hope. “System kabhi theek nahi hoga, aur kisi ko humara dhyan nahi aayega (The system is never going to get fixed and they are never going to pay attention to us),” he says with a voice tinged with pain.
The anger against hospitals is not just confined to the TB-infected HCWs; the families of those who lost the battle with the disease are equally angry. “After my husband was detected with TB, his condition kept deteriorating. They [hospital] never treated him properly. He’s gone now and I have nothing left. I only got the gratuity money, which is already over. There is no pension or compensation for the death of my husband for me. I even requested the hospital administration for a job but they refused to listen,” says Rajbala, whose husband Devender Kumar died of TB contracted at workplace.
Devender had got a job as a ward boy in the NITRD in 1990. Some 12 years later he was detected with MDR-TB; he died in 2015. Rajbala says that her husband would not get salary for medical leave he had to take for treatment and the family had no money for buying medicines regularly.
In fact, the employee union of the Delhi hospital had taken the issue to the health minister in 2000. They wanted the government to provide compensation to class-IV workers and their families in cases of infection and death. “Even though compensation of Rs. 2.5 lakh for TB-infected patients and Rs. 5 lakh for families of the deceased was allowed for, while preparing the records of TB patients we realised that those who had applied did not have TB and those who had the disease were nowhere to be found in the records. Later, there was also interference from the management. So, the issue was never resolved,” says Shambhu.
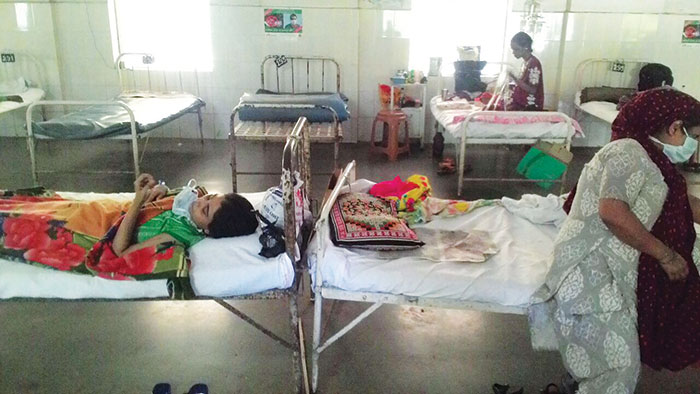
Patients rest at a GTB hospital ward
Obviously, the figures don’t match up. As per Dr Khaparde’s assessment of a high rate (50 percent) of TB-infected hospital staff, official numbers from the GTB hospital paint a different picture. In its screening of as many as 866 staff members (from June 2011 till March 2016), only 68 were diagnosed with TB. Going by the hospital records, there have been 18 deaths in the past five years. The hospital figures also show a decline in TB infection cases – in 2013, 25 new HCWs were diagnosed with TB, a year later the number was 12 and in 2015 the number was nine. These claims are questionable, as according to Dr Nanaware, the GTB hospital witnesses six deaths every day. Another doctor at the hospital, who does not want to disclose his name, says that on average 4.7 deaths took place every day at the hospital in 2015; even those who were being treated died and this is not being publicly accepted.
But in Delhi, doctors are not even ready to disclose the figures, given that they keep a record. GK Khurrana, general secretary of the Delhi Nurses Union, admits the hospitals are wary of this. “They don’t want to wash their dirty linen in public. I can’t say about TB hospitals but in general hospitals, they don’t hold any annual checkups for us. No counseling is done. When patients develop symptoms, they first visit a general hospital. By the time they are diagnosed with TB, the HCWs dealing with them have already caught the infection.”
Shambhu Kumar Singh agrees with Khurrana. “The management will never disclose the exact data. Most of the staff members have been infected with TB and many have even died. There are no checkups or counseling. In fact, as soon as sweepers and ward boys show symptoms, the management keeps telling them that there is nothing wrong with them, and refuse to test them. They only get admitted when their condition worsens,” he says.
It is high time that the prescribed and expected infection control measures are adopted by hospitals before their own staff take up more beds than outside patients. The WHO and the centre have already published guidelines comprising detailed technical and operational measures for reducing transmission of TB among HCWs.
Moreover, according to the Centers for Disease Control and Prevention, a leading public health institute of the US, it is the management’s responsibility to reduce the risk of infection among HCWs who are in direct contact with TB patients. Some of its important guidelines include ensuring proper cleaning and sterilisation of potentially contaminated equipment, training and educating HCWs regarding TB with specific focus on prevention, transmission, and symptoms and also screening of these HCWs to keep a check on infection.
Universally, too, it is recommended that patients need to be educated on minute things like cough etiquette to minimise the spread of infection. Segregation of patients with infectious TB is also important in preventing the spread in hospitals. Be it a general hospital or a TB hospital, all TB suspects should be provided a separate waiting area and they should be considered for quick priority service.
But given the apathy among the administration, the Mazdoor Union in Mumbai is now planning to move court. “The government has not adopted suggestions of the infection control committee. Besides, the number of workers dying due to infection is increasing,” says Narkar. He adds that the union is demanding inclusion of portable sterilisation machines, use-and-throw pouches for sputum, six-foot distance between beds on all four sides in wards, six-hour work shift for the staff and better quality high-protein diet.
Dr Nanaware, however, says that things have changed with the hospital starting a 12-point infection control programme. Provision of free TB treatment, protein supplements to healthcare workers for boosting immunity before returning to duty, N-95 masks, health education counselling, quarterly medical examination, patient segregation, special TB leave are some of the initiatives.
Dr Gita Nataraj, too, speaks of the administration’s achievements. “With the help of Centers for Disease Control and Prevention, US, we brought in measures since 2012. Screening of TB patients through sophisticated machines and clinical suspicion of respiratory infection is carried out for all workers quarterly. If TB is detected, appropriate treatment is given to patients. They are also tested for diabetes as it increases chances for acquiring TB.”
She adds: “Separate wards have been allocated for drug-resistant TB patients and all healthcare workers are provided with N-95 respirators once in two days as per the policy. Lab workers who handle culture are provided with these masks every day and there is no dearth of these respirators now. Sputum is disinfected with phenol and sodium hypochlorite, which are recommended for deactivating TB basicili, and windows have been opened up for more ventilation.”
Despite unfurling the list of accomplishments by hospitals and administrations, a lot more is required. Dr Lalit Anande, chief medical officer at GTB hospital, points out some of the shortcomings. Dr Anande, who has worked as a surgical registrar in the thoracic surgery department of the GTB hospital for 20 years, says, “Surgery which was the golden rule at one time is being overlooked by the government. When TB becomes drug-resistant, much can be managed with surgery which is not being done at all. With only five trained thoracic surgeons doing day and night surgeries, the cardiovascular and thoracic surgery (CVTS) branch of the hospital is concentrating only on cardiovascular and not thoracic surgery. The requirement for a thoracoscope to conduct surgery has been pending for several years now. Moreover, there is non-availability of a ventilator at the intensive respiratory care unit of the hospital.” Dr Anande, however, adds that as CVTS is a difficult study and takes years to master, it is not so lucrative and thus there is lack of trained doctors.
In terms of nutrition too, Dr Anande feels that “we have failed as an organisation”. “We just spend Rs. 25 daily on workers’ food. Where Bangladesh, Nepal and Pakistan are following the WHO-provided daily therapy, here alternate day therapy is being followed.”

Group of Tuberculosis (GTB) hospital in Sewree, Mumbai
Prakash Devdas says that it is the doctors who are not able to convince the municipality. As a case in point, he says, “If the doctors had asked for Rs. 200 for their daily food intake, they [municipality] would have gone down to Rs. 100. But if they are going to ask for Rs. 30, then obviously they will get Rs. 25 only.”
Dr Anande also blames doctors who are ignorant and do not refer cases at the right time. “In a confluence of treatment, there must be cross-reference so that patients are not left to die a slow and prolonged death. Also, despite availability of medicine and treatment, the government is not targeting the latent TB population.”
Dr Anande, who runs a community-based campaign called ‘May I Help You’ to educate people on the importance of nutritious diet and prevention from TB, adds that nearly 98 percent of anti-TB drugs manufactured by Indian pharmaceuticals are sold to the WHO. Through his campaign, the doctor gives lectures to school and college students, at corporate offices, railway platforms and religious places.
Throwing light on another issue, Devdas says that money too is not in the right hands. “It is the accounts section [of the BMC] that decides money allocation for government and municipal hospitals. It raises queries on the proposals that land on its desk. After getting the replies, the proposals are forwarded to the municipal corporation which again makes some more queries. The proposal then goes back to the concerned person. While all this goes on, the chief medical officer or the medical superintendent who does the ground work remains a mute spectator as they do not have the powers to allocate money.”
A staff member from the GTB hospital’s administration sympathises with the ordeals of TB patients. “When an earning member in a family gets infected with TB and is also harassed to receive his medicines, leave or payment, how does he take care of his family’s needs? He goes into depression and is forced to come to work in sickness. His health deteriorates further and it’s nothing but a slow death,” says the staff member. Dr Anande supports the views of the staff member by telling us that the hospital had to recently install grills [where required] after patients started committing suicide by jumping off higher floors.
Indeed, a perusal is required on the present condition of the hospital staff and its management. Dr Christopher succinctly sums it up, “It is possible that the measures were taken earlier [but they later turned lackadaisical]. They [authorities] have to now look back at all the measures.”
Some of the patient’s names have been changed to protect their identity.
sakshi@governancenow.com
geetanjali@governancenow.com
(The story appears as cover in June 1-15, 2016 issue of Governance Now)
As many as 1,351 candidates from 12 states /UTs are contesting elections in Phase 3 of Lok Sabha Elections 2024. The number includes eight contesting candidates for the adjourned poll in 29-Betul (ST) PC of Madhya Pradesh. Additionally, one candidate from Surat PC in Gujarat has been elected unopp
The provisional figures of direct tax collections for the financial year 2023-24 show that net collections are at Rs. 19.58 lakh crore, 17.70% more than Rs. 16.64 lakh crore in 2022-23. The Budget Estimates (BE) for Direct Tax revenue in the Union Budget for FY 2023-24 were fixed at Rs. 18.
The much-awaited General Elections of 2024, billed as the world’s biggest festival of democracy, began on Friday with Phase 1 of polling in 102 Parliamentary Constituencies (the highest among all seven phases) in 21 States/ UTs and 92 Assembly Constituencies in the State Assembly Elections in Arunach
Fit In, Stand Out, Walk: Stories from a Pushed Away Hill By Shailini Sheth Amin Notion Press, Rs 399
The recent European Union (EU) policy on artificial intelligence (AI) will be a game-changer and likely to become the de-facto standard not only for the conduct of businesses but also for the way consumers think about AI tools. Governments across the globe have been grappling with the rapid rise of AI tool
The Indian Railways is celebrating 171 glorious years of its existence. Going back in time, the first train in India (and Asia) ran between Mumbai and Thane on April 16, 1853. It was flagged off from Boribunder (where CSMT stands today). As the years passed, the Great Indian Peninsula Railway which ran the





